Lumbar Spinal Fusion
Up to 90% of patients experience pain relief with San Francisco Lumbar Spinal Fusion.
Pain after TLIF specifically is reduced 60-70 percent on average.
A San Francisco lumbar spinal fusion is a type of back surgery that can be done as an open, minimally invasive or mini-open procedure.
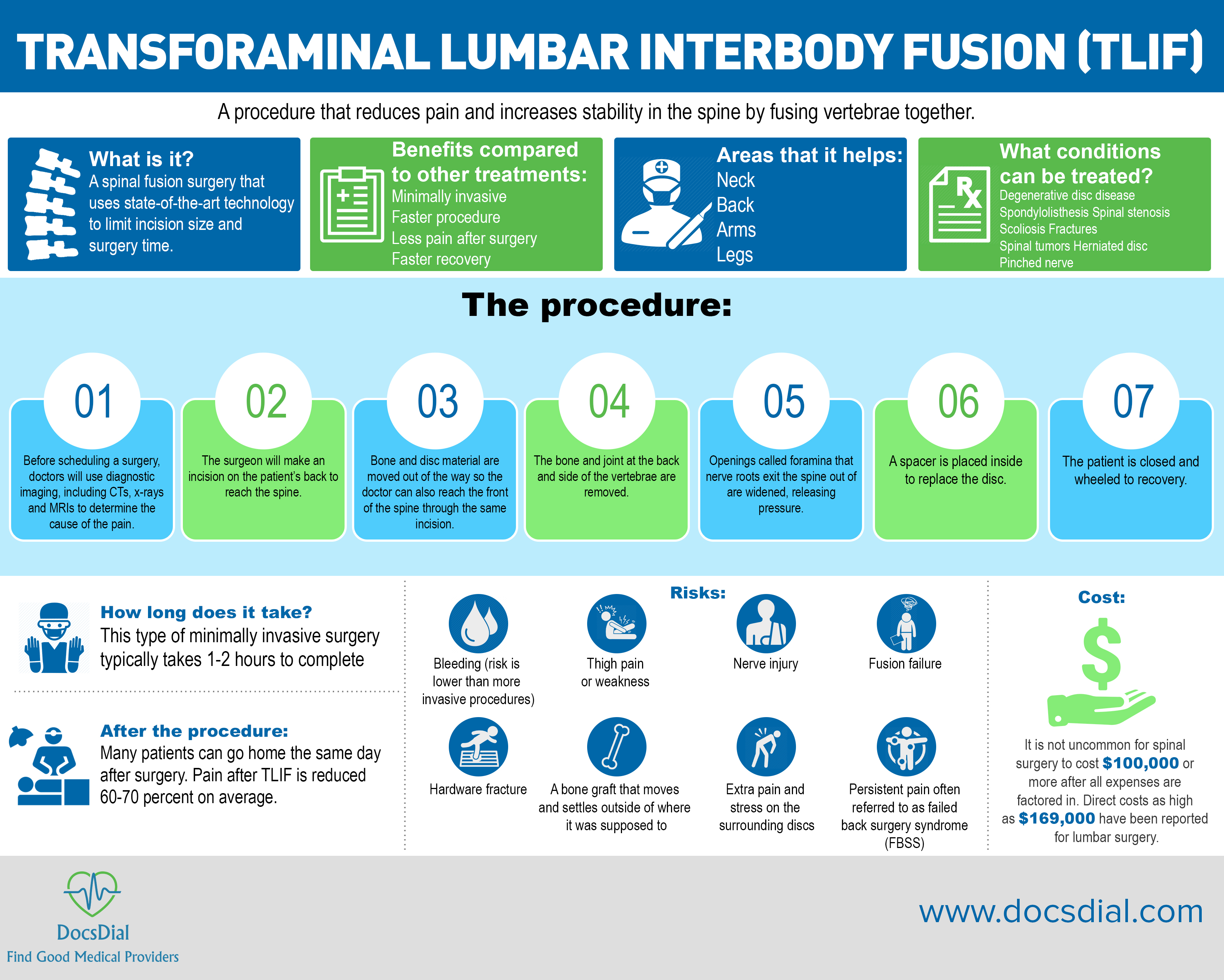 The procedure combines two or more vertebrae through a welding-like process in order to reduce pain and increase stability in the spine. It is used to treat chronic neck and back pain that may radiate to the arms and legs. People who suffer conditions such as degenerative disc disease, spondylolisthesis, spinal stenosis, scoliosis, fractures and spinal tumors in San Francisco typically make good candidates for the procedures. When possible, some spinal fusion surgeries can be done as outpatient procedures with minimal cutting and operating time—they are called minimally invasive spinal fusions. Depending on which vertebrae are causing pain and where potentially diseased discs are located, a fusion can be done on the thoracic (upper back) or lumbar spine (lower back).
The procedure combines two or more vertebrae through a welding-like process in order to reduce pain and increase stability in the spine. It is used to treat chronic neck and back pain that may radiate to the arms and legs. People who suffer conditions such as degenerative disc disease, spondylolisthesis, spinal stenosis, scoliosis, fractures and spinal tumors in San Francisco typically make good candidates for the procedures. When possible, some spinal fusion surgeries can be done as outpatient procedures with minimal cutting and operating time—they are called minimally invasive spinal fusions. Depending on which vertebrae are causing pain and where potentially diseased discs are located, a fusion can be done on the thoracic (upper back) or lumbar spine (lower back).
What is it?
San Francisco spinal fusions prevent pain associated with movement by fusing together two or more vertebrae in the spine to prevent painful movement. The pieces are welded together using a bone graft, made from either a cadaver bone or taken from the patient. These grafts are commonly referred to as cages. To be effective, Dr. Abbi has to be able to tell which vertebrae are causing the problems, so before scheduling a surgery they will use diagnostic imaging, including CTs, x-rays and MRIs to determine the cause of the pain. Without this knowledge, a spinal fusion is not typically recommended. There are two types of minimally invasive spinal fusions that target the lumbar spine—transforaminal lumbar interbody fusion, or TLIF, and lateral lumbar interbody fusion, called LLIF or XLIF. A transforaminal lumbar interbody fusion is used when Dr. Abbi needs to access both the front and back of the spine during the procedure. In addition to fusing the bones together with a bone graft, the surgery decompresses the spinal cord and/or spinal nerves and provides stability to the spine. There are several levels to this surgery. The first is called an open procedure and is not minimally invasive. There is also a minimally invasive version that uses smaller incisions and instruments to access the spine through, offering benefits including less pain post-surgery and shorter recovery times. In between these two approaches is the mini-open, which uses some of the minimally invasive techniques but not all of them, offering a middle ground in cases where a true minimally invasive surgery cannot be done. The other procedure—the lateral lumbar interbody fusion—uses a one-inch incision in the side of the waist to achieve the spinal fusion. After the damaged disc is removed, Dr. Abbi replaces it with a bone graft that acts as a spacer and helps the bone fuse together. If instability is of major concern, the surgeon may place a plate and screws into the spine as well to hold the spine steady and promote healing. In some cases an additional incision is made from the back (posterior) to insert stabilizing equipment. The surgery is performed by a neurosurgeon or orthopedic surgeon with special training in minimally invasive surgery and typically takes 1-2 hours to complete.Purpose
The main purpose of lumbar fusion is to reduce pain and create more stability in the spine. There are many options for San Francisco back pain sufferers. LLIF and TLIF is to reduce or eliminate pain in San Francisco back, arm and/or leg pain sufferers caused by movement in the spine. It was created as a minimally invasive alternative to other spinal fusion surgeries. With its smaller incision there is less potential for damage of nerves, blood vessels and organs. In an LLIF, instead of using normal instruments, tubular instruments are passed through the small space using a tunnel formed by the surgeon between the patient's abdominal organs and the spine muscles. In the TLIF, both parts of the spine are able to be worked on from one incision eliminating additional risks and a second incision site that can cause post-operative pain. Many patients prefer the lateral or transforminal approach to anterior or posterior interbody fusion procedures because they can go home the same day and recovery is shorter. Open and mini-open procedures find the same results for patients with a different approach. Dr. Abbi will recommend the best procedure for you.Benefits
The biggest benefit of San Francisco lumbar fusion surgery is pain relief. Whether it is complete or partial, most patients experience improvement in pain as well as becoming better able to perform daily tasks due to the reduction in pain. In most cases, patients do not notice the limited movement caused by fusion because they couldn’t move without pain before. This pain is commonly caused by other ailments that affect the spine such as a pinched nerve, degenerative disc disease, degenerative scoliosis or a herniated disc. Most patients report lower pain levels post surgery, as well as the ability to function better in daily life and perform normal activities. Other benefits include correcting mild to moderate scoliosis, relieving radiating pain and sensations such as numbness, weakness or tingling in the arms and legs, less stiffness upon walking or standing and being able to go home the same day as surgery thanks to the minimally invasive outpatient procedure. Minimally invasive surgery often causes less tissue trauma, less scarring and less postoperative discomfort, plus it requires shorter hospital stays.Areas the Surgery Helps:
San Francisco lumbar fusion surgery relieves pain in the lumbar spine, neck, back, arms and legs.What conditions can be treated?
San Francisco lumbar fusion surgery helps those who suffer degenerative disc disease, spondylolisthesis, spinal stenosis, scoliosis, fractures and spinal tumors.The procedure:
Lumbar fusion surgery can take anywhere from 2.5-7 hours often depending on how many levels of fusion must be done. The minimally invasive version takes 1-2 hours.- Before scheduling surgery, Dr. Abbi will use imaging machines to determine which vertebrae to operate on.
- The patient will be given general anesthesia before the procedure.
- Abbi will make an incision on the patient’s back to reach the spine
- In minimally invasive procedures, bone and disc material are moved out of the way so the doctor can also reach the front of the spine through the same incision. In open procedures a second incision will be made from the front.
- Abbi removes the bone and joint at the back and side of the vertebrae.
- Abbi widens the foramina that nerve roots exit through.
- A spacer is placed inside to replace the removed disc.
- Bone grafts or metal plates are used to fuse the spine together.
- The patient is closed and wheeled to recovery.
Risks
Every surgery includes the following risks: bleeding, infection, blood clots and reactions to anesthesia. Lateral lumbar interbody fusion and transforaminal lumbar interbody fusion have their own risks, but they are limited due to the small incision and short operating time. Bleeding, especially, is of less concern. Other complications include: thigh pain or weakness that lasts weeks to months, nerve injury, abdominal organ injury (LLIF), fusion failure (meaning the graft didn’t effectively fuse the vertebrae into one bone), hardware fracture, a bone graft that moves and settles outside of where it was supposed to, extra pain and stress on the surrounding discs and persistent pain often referred to as failed back surgery syndrome, or FBSS.After the procedure:
Patients should anticipate some pain following San Francisco lumbar fusion surgery, and it can take 3-12 months for a full recovery. After the procedure patients should undergo physical therapy to regain strength and range of motion as well as schedule a follow-up appointment 4-6 weeks after.Alternatives
Back surgery is almost never recommended unless other methods have failed first. Before resorting to even this minimally invasive procedure, Dr. Abbi will try a mix of other interventions including pain medication, physical therapy, other physical modalities possibly including massage or acupuncture and sometimes steroid shots in the spine to relieve pain. If lumbar fusion is needed, there are several types of spinal fusions available. LLIF and TLIF are often preferred for their small incisions and short operating times but they aren’t always a good fit for candidates. Instead, anterior lumbar interbody fusion, posterior lumbar interbody fusion or another type of spinal fusion surgery may be recommended to treat vertebrae and damaged discs in the lumbar spine.Payments/cost
It is not uncommon for spinal surgery to cost $100,000 or more after all expenses are factored in—the surgery, recovery, physical therapy, diagnostic imaging, medication and disability. Direct costs as high as $169,000 have been reported for lumbar surgery. Where you have the surgery and who performs it will also affect cost. Insurance, luckily, often covers all or part of the surgery. Check with your provider for an accurate estimate, and don’t forget to factor in aftercare.References:
"Back Surgery: Too Many, Too Costly and Too Ineffective." Common Exercise Mistakes. June 01, 2011. Accessed May 05, 2018. http://www.toyourhealth.com/mpacms/tyh/article.php?id=1447. "Spinal Fusion: Lateral Lumbar Interbody Fusion (LLIF)." , Hemorrhagic Stroke. Accessed May 05, 2018. https://www.mayfieldclinic.com/pe-llif.htm. "Lateral Lumbar Interbody Fusion (XLIF) Video." Spine-health. Accessed May 05, 2018. https://www.spine-health.com/video/lateral-lumbar-interbody-fusion-xlif-video. Laser Spine Institute. "Lateral Lumbar Interbody Fusion | Minimally Invasive Stabilization (MIS) Options for Lumbar Spine." Laser Spine Institute. Accessed May 05, 2018. https://www.laserspineinstitute.com/spinal_orthopedic_procedures/llif/. Montgomery, Stephen P. "TLIF Back Surgery Success Rates and Risks." Spine-health. Accessed May 05, 2018. https://www.spine-health.com/treatment/spinal-fusion/tlif-back-surgery-success-rates-and-risks. Mudbug. "Spinal Fusion: Do You Really Need One?" Michael A. Gleiber, MD. April 20, 2015. Accessed May 05, 2018. https://michaelgleibermd.com/news/really-need-spinal-fusion/. Transforaminal Lumbar Interbody Fusion (TLIF) – The Spine Hospital at The Neurological Institute of New York." The Spine Hospital at The Neurological Institute of New York. Accessed May 05, 2018. http://columbiaspine.org/treatments/transforaminal-lumbar-interbody-fusion-tlif/Fusion is a surgical technique in which one or more of the vertebrae of the spine are united together (“fused”) so that motion no longer occurs between them.The lack of motion helps to decrease the back pain. Bone grafts are placed around the spine during surgery. The body then heals the grafts over several months – similar to healing a fracture – which joinsthe vertebrae together. Spinal fusion can help in the correction of deformity (spinal curves) the treatment of instability (spondylolisthesis) or management of painful intervertebral discs (degenerative disc disease). A spinal decompression is a procedure to remove pressure form compressed (pinched) nerves. This includes removing bone or soft tissue that is causing the pressure on the nerves. Once all the compressed nerves are alleviated of compression, the leg pain usually improves. This removed bone is then used as the bone graft to help the spinal fusion. This procedure (called laminectomy) is often done together with a fusion.
